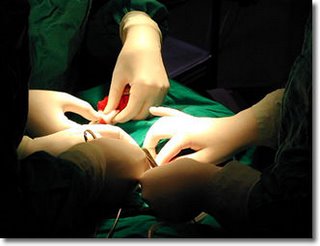
OK, now I’ll come down from the stratosphere of story theory and up from the adaptive unconscious back to ground level and the straight-forward business of surgery.
Today was the pre-surgical clinic session at Grand River Hospital. To prepare for this session, I had to bring in a form for admission to surgery and a form for the anaesthesiologist, a list of medications, and the containers for each of the medications I’ve had to take since the beginning of the year. I had to have an electrocardiogram, a blood pressure test, and blood samples taken.
The nurse who provided orientation outlined everything that I should expect in undergoing a low anterior resection. We talked about oxygen masks, catheters for liquid waste, tubes in the nose to help remove gastric juices in the stomach, and a possible drainage tube from the vertical incision to help drain the abdomen. Not a pretty sight.
After I am back in the ward, there will be breathing exercises to be performed with a special device every hour, a little exercise each day, beginning with dangling my feet over the edge of the bed, progressing on to a walk from the bed to the door and back again the next day, maybe down part of the hallway the next day, and so on. I’m planning on making it down to the radiation treatment area in the cancer centre by the fifth day to see the therapists who treated me for 5 ½ weeks.
The lengthy 8 days of hospitalization is mainly because bowel surgery requires very careful control of fluid and food intake, the key milestone of which will be the first bowel movement after surgery. That in itself takes a long time since I will not ingest fluids from Monday night at midnight until Friday. There will be intravenous fluids, of course, but no ingestion of anything more than sucking on ice chips for the first three days. After that, they will introduce low-residue foods very slowly and carefully, attempting to give the bowels as much opportunity to heal before getting back to work as possible.
One good thing, I guess, is a device that administers something called Patient Controlled Analgesia, a type of pain relief in which the patient rather than the nursing staff gets to decide when the next dose of pain reliever is administered. The amount is monitored by the nursing staff. The nurses will let me know whether I need to use it more frequently or less frequently.
Now, what about watching the Final Four on TV? I may be well enough to rent a television for the final four NCAA basketball championships in early April.

No comments:
Post a Comment